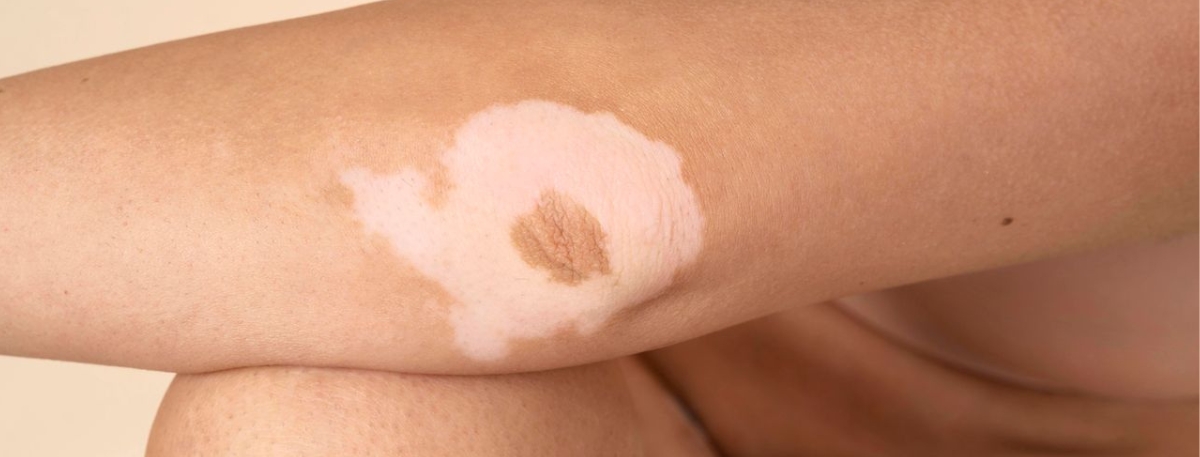
Vitiligo is a skin condition that affects pigmentation when melanocytes, the cells responsible for skin color, are damaged or stop functioning properly. In children, vitiligo can be particularly challenging, not only because of its visible appearance but also due to its emotional and social impact during critical developmental years.
Understanding vitiligo medication options and the role of clinical research helps families make informed decisions about pediatric dermatology care. At PedSkin Research, families can learn about vitiligo in children, available management approaches, and ongoing clinical research designed specifically for pediatric patients.
Understanding Vitiligo in Children
Vitiligo is considered an immune-mediated condition. The immune system mistakenly targets melanocytes, leading to areas of depigmented skin. These lighter patches may appear anywhere on the body, including the face, hands, feet, scalp, and around the eyes or mouth.
Vitiligo can develop at any age, but a significant number of cases begin during childhood or adolescence. The progression of vitiligo varies widely. Some children experience slow changes over time, while others notice more rapid development of new patches.
Vitiligo is not contagious, and it is not caused by hygiene, diet, or direct skin injury alone. While genetics may play a role, the exact cause remains an active area of medical research.
Common Types of Pediatric Vitiligo
Pediatric dermatologists may classify vitiligo into several patterns, including:
- Non-segmental vitiligo, which often appears symmetrically on both sides of the body
- Segmental vitiligo, which affects one area or side of the body and may stabilize earlier
- Localized vitiligo, involving a limited number of patches
Understanding the pattern helps guide monitoring and management strategies.
How Vitiligo Is Diagnosed in Children
Diagnosis is usually made through a clinical examination. Pediatric dermatologists evaluate:
- Skin appearance and distribution of depigmentation
- Onset and progression of patches
- Family history of vitiligo or autoimmune conditions
In some cases, specialized light examination tools may be used to help visualize pigment changes more clearly. Laboratory testing is not routinely required unless there is a clinical reason to evaluate for associated conditions.
Vitiligo Medication Options for Children
There is currently no single medication that works for every child with vitiligo. Pediatric vitiligo treatment focuses on managing immune activity, supporting repigmentation when possible, and maintaining skin health.
Medication options may include:
Topical Corticosteroids
These medications are sometimes used to help reduce localized inflammation and immune activity in affected areas. Pediatric dermatologists carefully select strength and duration to balance effectiveness and safety.
Topical Immunomodulators
Certain non-steroidal topical treatments may be used in sensitive areas such as the face. These medications aim to influence immune responses without thinning the skin.
Supportive Topical Therapies
Moisturizers and sun-protective measures play an important role in maintaining skin comfort and reducing contrast between affected and unaffected skin.
Medication selection depends on:
- Child’s age
- Location and extent of vitiligo
- Skin sensitivity
- Response to previous treatments
Light-Based Therapies and Vitiligo Management
In some cases, pediatric dermatologists may discuss controlled light-based therapies as part of vitiligo care. These approaches are administered under medical supervision and are tailored to minimize risks, especially in children.
Light-based treatments are not appropriate for all patients, and careful evaluation is required before considering this option.

The Importance of Individualized Pediatric Care
Children respond differently to medications than adults. Pediatric vitiligo care emphasizes:
- Age-appropriate treatment selection
- Gradual adjustments based on response
- Ongoing monitoring for skin tolerance
Pediatric dermatologists also educate families about realistic expectations, as repigmentation may be gradual and variable.
Clinical Research and Vitiligo in Children
Clinical research plays a vital role in expanding knowledge about vitiligo and improving care options for pediatric patients. At PedSkin Research, clinical studies explore investigational therapies aimed at better understanding immune pathways involved in vitiligo.
These studies focus on:
- Evaluating safety in pediatric populations
- Understanding how treatments affect developing immune systems
- Collecting data that may guide future pediatric dermatology standards
Participation in clinical research is voluntary and includes comprehensive screening, informed consent, and ongoing medical oversight.
Why Pediatric Clinical Trials Matter
Many treatments used in children are based on adult data. Pediatric clinical trials are essential to ensure:
- Treatments are appropriate for children
- Safety profiles are well understood
- Dosing and protocols reflect pediatric needs
Families who participate in research contribute to medical progress while receiving structured follow-up and education.
Emotional and Psychological Impact of Vitiligo
Vitiligo can affect a child’s self-image, particularly when patches appear on visible areas such as the face or hands. Children may experience:
- Self-consciousness or embarrassment
- Social anxiety or questions from peers
- Emotional stress related to appearance changes
Pediatric dermatology care recognizes the importance of addressing emotional well-being. Parents can support children by encouraging open communication and focusing on strengths beyond physical appearance.
Sun Protection and Daily Skin Care
Children with vitiligo benefit from consistent sun protection. Depigmented skin lacks natural pigment protection, making it more sensitive to sun exposure.
Daily care recommendations often include:
- Broad-spectrum sunscreen use
- Protective clothing when outdoors
- Gentle skin care routines
These measures help protect skin health and reduce visual contrast.
Long-Term Outlook for Children with Vitiligo
Vitiligo is often a long-term condition, but its course is unpredictable. Some children experience periods of stability, while others may notice gradual changes over time.
With proper dermatology care, education, and emotional support, many children adapt well and maintain a positive quality of life.
Learn More About Pediatric Vitiligo Research
Children diagnosed with vitiligo may qualify for clinical research studies depending on age, diagnosis, and study criteria. Educational resources and research opportunities help families understand available options without obligation.
Our Location
Coral Gables
4425 Ponce de Leon #115, Coral Gables, FL 33146, United States
Nearby Cities:


Request An Appointment
To request an appointment, please fill out the contact form below. Our team will get back to you as soon as possible to confirm your appointment and answer any questions you may have.
We look forward to assisting you.
Meet Our Medical Director
Mercedes E. Gonzalez M.D.
Dr. Mercedes E. Gonzalez is a board-certified pediatric dermatologist. After graduating from Emory University, she earned her degree at Rutgers–New Jersey Medical School in 2004. Always drawn to working with children, she accepted the prestigious pediatrics program at the Morgan Stanley Children’s Hospital of New York–Columbia University where she solidified her interest in treating skin disorders. She then completed a dermatology residency followed by a clinical fellowship in pediatric dermatology at the top-ranked New York University (NYU) Department of Dermatology.
Her gentle, child-friendly bedside manner, combined with her broad knowledge of childhood skin diseases and their treatments, make her the preferred pediatric dermatologist in Miami. In addition to practicing medicine, Dr. Gonzalez currently serves as a clinical assistant professor at The FIU Herbert Wertheim School of Medicine and The Phillip Frost Department of Dermatology at Miller School of Medicine.
Dr. Gonzalez serves as the Principal Investigator on numerous clinical trials and has a special interest in severe skin disease in children. She lectures regularly at Dermatology conferences and to medical students and residents and is the co-editor of 3 dermatology textbooks, including the recently published 2nd edition of Goodheart’s Same Site Differential Diagnosis, and has published over 50 journal articles.

